Why is this website called “Don’t Go to the Ouch!”?
 Many people have asked me why I called the website Don’t Go to the Ouch!
Many people have asked me why I called the website Don’t Go to the Ouch!
Physically, we may look different but ‘under the skin’….we are pretty much the same.
Our bodies are comprised of different tissues – soft and hard – including muscles, joints, bones, fascia, nerves and blood vessels. And each of these structures can cause different types of sensations (feelings) when they are irritated, injured, or damaged in some way.
But when we say OUCH depends on many factors – including what that discomfort means to us, how we have learned to experience and understand different painful sensations, and whether or not that feeling is dangerous or feels like it is dangerous.
It may be interesting to note an early experiment on pain perception.
The experiment involved asking university students to place their forearm in cold water (yes, it was icy cold), and to keep it in the water for as long as possible. The students knew that it was ONLY cold water. The investigators were interested in finding out how long it took each student to take their forearm out of the water … when did they say ‘ouch’ or ‘enough’!
(I am uncertain if they were also asked WHY they took their forearm out of the water.)
Some students took their forearm out of the water almost immediately ‘ because they did not like the feeling (or was there any fear attached to it as well?). Others kept their forearm in the water until their skin was nicely discoloured.
So, what does this early experiment on pain perception tell us? Even though the cold water was not going to cause anything serious or dangerous to happen, it did cause some type of response/reaction in some students (fear? a memory? a stressful time with water?)
Understanding how the physical sensation of ![]() is transmitted to our brain and when/why we say OUCH may help us better understand what and how we interpret the different sensations we are experiencing … and decide what is dangerous — in that it requires further investigation – vs what is just annoying – but still needs some attention.
is transmitted to our brain and when/why we say OUCH may help us better understand what and how we interpret the different sensations we are experiencing … and decide what is dangerous — in that it requires further investigation – vs what is just annoying – but still needs some attention.
How we respond to that feeling nonetheless, is up to us – and is often a learned behaviour. What can I do about it? What choices do I have? What does this sensation mean now? and for my future? Does it mean that I cannot go back to work or return to my sports/hobbies?
OUCH (even if you do not say it out loud) can also be a message that says: I need to stop that exercise/that movement/the weight is too heavy/I do not want to hurt myself. (We will discuss exercise and movement in the next OUCH blog).
Though there are times when ![]() can be experienced with no obvious visual injury or problem, pain more frequently starts in a very physical way.
can be experienced with no obvious visual injury or problem, pain more frequently starts in a very physical way.
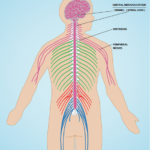
The brain and spinal cord are continuous with each other. Nerves exit the openings in the vertebral column (foramina, facet or vertebral joints) and travel down our arms and legs and throughout our body.
Different nerves innervate the viscera – the deeper structures, the internal organs (spleen, gut, kidneys, heart etc.).
In fact every part of our body is innervated by some type of nerve ending or structure.(Reminder that there is a video titled “The Nervous System” posted on the first blog.)
Nociceptors are sensory receptors found in and around all of the tissues in our body, including, muscles, joints, periosteum (the soft covering of our bones), vertebral discs and nerves. They can send different types of painful messages – to the brain – where that message is ‘processed’ or interpreted.
Different receptors – respond to different forces – such as pressure, vibration, thermal (hot and cold), stretch and proprioception.
Trauma (injury), concussion, medical conditions (fibromyalgia, migraines) disease (cancer) can cause changes to the usual nerve pathways, creating very confusing pain sensations. As a result, it is often more difficult to ‘control’ the different sensations.
Information on fibromyalgia, osteoporosis, stress, concussion (acquired brain injury), soft tissue pain, neck and back spinal pain are noted briefly under Special Topics.
Physical Therapist (American delineation) Kathleen Sluka, PT, PhD, FAPTA, has edited and authored many chapters in a comprehensive text titled Mechanisms and Management of Pain for the Physical Therapist. (Second edition available from Wolters Kluwer)
Using the IASP (International Association for the Study of Pain) framework, Kathleen and her co-authors include current information on several key titles 1) Basic Concepts and Mechanisms 2.) Physical Therapy Pain Management 3.) Interdisciplinary Pain Management, and 4.) Pain Syndromes (including case studies). This text is recommended for all health providers treating/managing the patient with acute and chronic pain. You do not have to be a physiotherapist to appreciate its contents.
TAME THE BEAST: It’s time to rethink persistent pain is a 5-minute video developed by physiotherapy colleague Lorimer Moseley. PT, Ph.D.
It is both entertaining and educational, though it does help if you speak Australian English!
Thanks for reading! Your comments and ideas are appreciated
Please contact me at gloria@dontgototheouch.com
Coming up next: Exercise – or should we title it — How do I move when I am in Pain?

